This video is a segment of the 2022 BRAIN HEALTH Educational Series published at the IPHA/Health & Healing 101 Report. The program presents interviews about Post Concussive Syndrome from health professionals and advocates detailing the diagnostic protocols for acute and chronic sports related injuries plus an overview on the current findings about mental disorders associated with head trauma.
POST-CONCUSSIVE SYNDROME 101
By: Dr.
Michael Gruttadauria
Most
people believe that you need to be knocked unconscious to have a concussion- and
that's just not the case. Even a “small” impact
injury, what they call mild traumatic brain injury or mild concussion affects
thousands and thousands of people every month. From falls accidents, sports, assaults-- many
different things can cause concussions.
Something called POST-CONCUSSIVE SYNDROME can happen from these
mild traumatic brain injuries that may appear to resolve themselves. As far as
the symptoms go, most people end up with headaches, blurry vision, dizziness or
lightheadedness. After about a week, these symptoms tend to usually go away.
But up to 30% of people have persistent symptoms. And those persistent concussion
symptoms can be the same things like headaches and dizziness, but it actually
can progress into anxiety and depression and changes in personality and so on.
This is really when we need to get involved.
The traditional recommendation and prevailing wisdom for a
long time was actually to just take it easy, stay in a dark room and rest--
don't do anything exertional and stay off the computer. Don't watch too much TV
and your brain will just heal. Lately,
we find that this is no longer the case. You may want have physiological rest,
but then what you really want to do is have ACTIVE rest, which is allowing the
brain to work- pushing the brain to work.
There are physiological changes that go on in the brain
when you have a trauma. When you have this initial injury (and depending on the
extent of the blow to the head), you have changes in the micro environment
within the brain. You also can have an actual bruise. You can have changes in
blood vessel diameter. You can have torn blood vessels. With concussion, most
of these things are invisible. MRI and
CT scans are usually negative- and patients are usually sent home from the ER
and told to rest. No follow ups are
assigned from this point, and this is where we need to do better.

HEAD IMPACT IN SPORTS
With high impact sports like boxing and football and
soccer, where you have repetitive blows to the head, there are studies that are
actually show that repetitive concussive forces can actually be additive. You
can have an additive effect. It doesn't have to be one giant impact where you
might see a wide receiver going over the middle and catching a soccer ball.
Getting violently laid out by a linebacker may not even be
as bad as the offensive and defensive linemen that are banging their heads
against each other for 60 plays a game, per se. We we're all differently
susceptible to concussion. Somebody could have what would appear to be a more
minor concussion and have greater symptoms for a longer period of time, as
opposed to a really significant concussion.
SYMPTOMATOLOGY:
The GUT-BRAIN CONNECTION
I had a 32 year old former professional hockey player see
me for ongoing symptoms that he related back to the multiple concussions that
he sustained from a game. He had been traveling around the world and had access
to the top doctors. Over time, he contracted persistent headaches, balance
problems and dizziness that really began affecting his life. It actually forced
him out of hockey.
Between his hockey career and his present life, he
self-medicated the compounded set of problems that just weren't going away. These
symptoms are never really looked at objectively because many physicians are not
necessarily equipped to look too deep for dysfunctions, diseases or damage this
complex. The patient ended up having a chronic gastrointestinal problem as well
as an inner ear problem. And these two things are more functional in nature. These
would not appear in an MRI or a CT Scan.
What we realized was that the GUT-BRAIN CONNECTION was so powerful. When
we put him on an anti-inflammatory diet and we did eye-based and balance-based
rehabilitation within two months, all of his symptoms disappeared.

In other patients, we look at the neurology, the
biochemistry, the inflammation, the gut and the microbiome. By fixing the microbiome and changing their
diet, experience has shown that all of their concussion symptoms go away. So if
we're not looking at the gastrointestinal system, we're literally missing 50%
of the problem.
FROM THE LAB: RESEARCH ON CONCUSSION IMAGING
10/1/2022- In collaboration the Bard Diagnostic Imaging (NYC), diagnostic imaging specialists, neurologists and neuropsychologists are now in the process of assembling a comprehensive set of mutli-modality diagnostic protocols and specific physiological scan points for the study of POST-CONCUSSIVE SYNDROME. This review covers the establishment of imaging base line studies and a formal analysis of hemodynamics that offer quantifiable evidence from non-invasive modalities.
One of the primary studies is the use of ultrasound technologies including the Transcranial Doppler for the Basilar Artery, the Extracranial Doppler for the Temporal Artery and the Transorbital Doppler for the ophthalmic and central retinal vessels. These areas of the head provide essential blood flow readings for the detection of abnormality from latent effects of potential impact.
“Looking at the arterial-venous ratio and getting baseline is a great tool. Then, doing functional neuro interventions to enhance frontal lobe function (like cerebellar stimulation with complex upper body movements or specific vestibular canal stimulation) can create changes in the AV ratio and show positive correlation with symptom reduction”, states Dr. Mike Gruttadauria in an earlier interview.
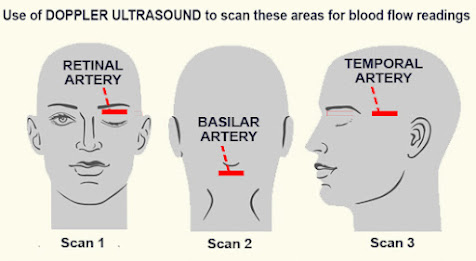
Dr. Robert Bard explains his prime strategy for scanning with ultrasound. "We need to position the probe to the lower/back of head- where the basilar
artery is available. This blood vessel supplies oxygen-rich blood to areas of
the brain and the autonomic/central nervous system. Next, we position the TCD probe to the temporal region, where temporal
artery is available. This is located just anterior to the ear, and is a guideline that
is used by most practitioners to examine blood flow to the brain &
measurement of cardiac cycle. We identify the heart rate or the pulse also
shows that the extracranial blood flow is intact as it goes towards the eye. Afterwards, we position a LINEAR probe to the OPTIC REGION- specifically to
study the optic nerve to show the paucity of the vessels in the central retinal
artery and choroidal vessels."
Clinical Spotlight: Concussion Management
10/16/2022- In a recent collaborative study of sports-related brain injuries, Dr. Alex Gometz (NYC) Founder Concussion Management of New York recently joined Dr. Robert Bard to conduct an investigative study about new imaging protocols recording pathologies of brain trauma. During this study, Dr. Gometz shared his clinical insights on concussion management with The Integrative Pain Healers Alliance (IPHA).
Meet Dr. Alex Gometz: Review on Athletic & Pediatric ConcussionDr. Gometz' practice is focused on the diagnostics and management of concussion in the athletic population and the pediatric community. During an exclusive interview, he reflected on the current guidelines covering patient analysis and the heavy pressure on professional athletes to return to play. "Obviously the league and fans want players to play. (I feel that) they need to have clearer guidelines based on better facts for the sake of the well-being of the player. I find that the current protocols may not be adequate, given the new research that shows recovery time may take longer. Studies show that protocols should be more sensitive to each player’s individual vulnerabilities. This is new research that should be taken into consideration and used to adapt the current protocols".
As an avid student of therapeutic advancements, Dr. Gometz is committed to staying on top of the latest clinical innovations and treatment modalities. On the care of MSK issues, regenerative therapies like PRP & EXOSOMES as well as non-invasive energy treatments like SHOCKWAVE, PEMF (Electromagnetic Field therapy), COLD LASER among others are well established in the market. But due to the fast paced progress of this industry, Dr. Gometz finds that not all practitioners are able to keep up with the latest innovations - especially when it comes to technologies that offer new ground in the resolution of concussion symptoms.

Disclaimer & Copyright Notice: The materials provided on this website/web-based article are copyrighted 2022 and the intellectual property of the publishers/producers (The NY Cancer Resource Alliance/IntermediaWorx inc and the AngioFoundation (501c3). It is provided publicly strictly for informational purposes within non-commercial use and not for purposes of resale, distribution, public display or performance. Unless otherwise indicated on this web based page, sharing, re-posting, re-publishing of this work is strictly prohibited without due permission from the publishers. Also, certain content may be licensed from third-parties. The licenses for some of this content may contain additional terms. When such Content licenses contain additional terms, we will make these terms available to you on those pages (which his incorporated herein by reference). This feature content and the digital platforms this resides in does not support, endorse or recommend any specific products, tests, physicians, procedures, treatment opinions or other information that may be mentioned on this site. Referencing any content or information seen, published or shared by other individuals is solely at your own risk. The publishers/producers of this article reserves the right, at its sole discretion, to modify, disable access to, or discontinue, temporarily or permanently, all or any part of this Internet web site or any information contained thereon without liability or notice to you.












No comments:
Post a Comment