10/16/2022- In a recent collaborative study of sports-related brain injuries, Dr. Alex Gometz (NYC) Founder Concussion Management of New York recently joined Dr. Robert Bard to conduct an investigative study about new imaging protocols recording pathologies of brain trauma. During this study, Dr. Gometz shared his clinical insights on concussion management with The Integrative Pain Healers Alliance (IPHA).
Dr. Gometz' practice is focused on the diagnostics and management of concussion in the athletic population and the pediatric community. During an exclusive interview, he reflected on the current guidelines covering patient analysis and the heavy pressure on professional athletes to return to play. "Obviously the league and fans want players to play. (I feel that) they need to have clearer guidelines based on better facts for the sake of the well-being of the player. I find that the current protocols may not be adequate, given the new research that shows recovery time may take longer. Studies show that protocols should be more sensitive to each player’s individual vulnerabilities. This is new research that should be taken into consideration and used to adapt the current protocols".
As an avid student of therapeutic advancements, Dr. Gometz is committed to staying on top of the latest clinical innovations and treatment modalities. On the care of MSK issues, regenerative therapies like PRP & EXOSOMES as well as non-invasive energy treatments like SHOCKWAVE, PEMF (Electromagnetic Field therapy), COLD LASER among others are well established in the market. But due to the fast paced progress of this industry, Dr. Gometz finds that not all practitioners are able to keep up with the latest innovations - especially when it comes to technologies that offer new ground in the resolution of concussion symptoms.
RECOVERY TIME AND CONTINUED MONITORING OF CONCUSSION PATIENTS
"It is imperative to constantly monitor progress of any concussion sufferer and it should be guided by current, objective testing and quantitative data", states Dr. Gometz. "You cannot rely purely only on symptoms to determine if the patient is getting better. Overall, people with a history of concussions, are more vulnerable to greater damage during future concussions. They tend to be more sensitive to lower amounts of pressure, causing similar symptoms".
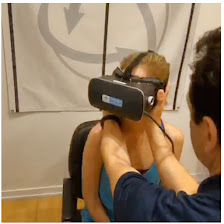 In the care of concussion cases, Dr. Gometz highlights one caveat; A player with a history of a single concussion that has fully recovered (as indicated by symptoms as well as quantitative data from specific tests) can be considered to be on equal footing with players with NO history of concussion. This comparison is based on the level of vulnerability to future injuries. Studies show that full recovery from a single concussion is effective at helping players bounce back to fairly equal health as they were prior. Players with a history of concussion without full recovery do not enjoy this benefit and a future concussion can happen with less amount of force, making them more vulnerable.
In the care of concussion cases, Dr. Gometz highlights one caveat; A player with a history of a single concussion that has fully recovered (as indicated by symptoms as well as quantitative data from specific tests) can be considered to be on equal footing with players with NO history of concussion. This comparison is based on the level of vulnerability to future injuries. Studies show that full recovery from a single concussion is effective at helping players bounce back to fairly equal health as they were prior. Players with a history of concussion without full recovery do not enjoy this benefit and a future concussion can happen with less amount of force, making them more vulnerable. Observing the common pattern in sports teams, athletes seem to return to the game sooner than non-pros. That may be due to the pressure from the organization and the player’s own drive to continue playing. This premature return contributes to setting premature standards that are clearly inadequate and potentially unrealistic. Standards need to include specific quantitative measures so that each player can demonstrate objective improvement. Schools should make sure their protocols are safe and reviewed by a medical board with proper steps and safeguards instead of copying other institutions’ protocols, following professional accountability.
MENTAL ISSUES FROM POST CONCUSSIVE DISORDER
Pre-existing mental conditions make the diagnosis and treatment more delicate. The underlying condition can challenge the client and healthcare provider to meticulously investigate the efficacy of each component of testing and treatment choices, timing, and tolerance. Certain preexisting mental health conditions can be characterized by similar dysfunctions caused by brain injury. On the side of treatment, some of those same conditions and understanding response to treatment can vary, fostering inaccurate expectations when it comes to recovery time. Another issue is the possibility of medications side effects that can also be similar to symptoms of a concussion, adding complication to the prognosis or discharge. Lastly, the availability of treatment choices can be greatly limited as some can be contraindicated- perhaps due to an abundance of precautions affecting clinical decision making.
“I find there to be a vast difference between adult cases and pediatrics as far as the complexity of the developing brain (pediatric). In this stage of development, the brain is undergoing the generation of new pathways that can be permanently disturbed”, says Dr. Gometz. “Overall, there appears to be a lack of professionals treating pediatrics in the field who are knowledgeable enough to discern the types the of treatment and management protocols. We advise parents to ‘never guess or think that your child is okay judging by current report of symptoms.’ A concussion is only considered mild or severe after the evaluation of objective and quantitative testing. The amount of force applied to the brain may cause disturbance to the neural mass in different levels and patterns that vary by individual. Experienced professionals try to use a wider set of analyses to detect the more silent and overlooked cases.”
Currently, there is growing concern that head injury evaluations and the follow-up care provided to patients often rely on outdated research. They may not be comprehensive enough, therefore lacking depth and focus on the most impactful priorities. More attention needs to be done to assist healthcare providers to acquire the tools and skills that can return the injured brain faster to relative normal function. This includes using multi-systems stimulation following clear guidelines.
JESI STRACHAM is a trauma survivor turned EMPOWERMENT COACH on a mission to help individuals see the opportunity in their obstacles. Jesi's injuries from a motorcycle accident (1/2015) included TBI/Traumatic Brain Injury and a spinal cord injury. Instead of accepting disability as her reality, Jesi's spirit to overcome her struggles made her one of the country's top advocates for wellness, empowerment, and improved lifestyle for all traumatic injury victims and wheelchair-bound individuals.
BRAIN/BODY WELLNESS PROGRAM & COPING WITH TBI
By: Jesi Stracham
I have a fitness community for wheelchair users called Wheel With Me Fitness and we talk a lot about nutrition. From my research and coursework on nutrition, I learned that we can educate ourselves about anything - especially thanks to the internet. We could find just about any resource on just about anything. For any athlete (per se) or any who suffers or multiple head traumas, should definitely pay attention to their nutrition, hydration, and sleep. This includes what they feed their brain, both physically and mentally.
I learned more about reducing inflammation in your body I was experiencing a lot of shoulder pain. This is when I found OMEGA-3’s and the power they have in reducing inflammation in our body. I use 1st Phorm’s Full-Mega. I use four a day. Full Mega not only improves my shoulder pain, but also my brain health as a whole. I've noticed a massive difference between when I do and don’t use my Omega-3 supplement and how well my brain funcitons. I notice toward the end of the day it becomes harder to form sentences and complete thoughts. I think that's really important that we stay mindful on the way both internal and external circumstances have on the way our body functions. We have to be mindful of how our brain acts at the end of the day- and I’ve noticed in my own body this has a lot to do with what we're eating. In relation to my brain my Omega-3 supplements are a big go to for me, but as I’ve researched I also have added Avocado, Blueberries, Broccoli, and more water more frequently. I think a lot of people don't take the time to really pay attention to their body and what their body's telling them.
SLEEP HYGIENE
Sleep is important to the way your brain recovers. Sleep hygiene is really important to the quality of your sleep. Start by having a cool, dark room with no lights and no technology. It's important to have a nighttime routine so your body can start producing melatonin. I've noticed that if I don't stick to my nighttime routine, I typically don’t get quality sleep. Prepping for sleep is crucial; limiting screen time and phone chats is a good start. Residual effects from these things tend to linger in your brain- and are not constructive.
I also have a morning routine. I use a sunrise alarm, which I love because it wakes me up peacefully with the gradual light mimicking the sun, and soft sounds. When I get up, I read my devotion, I read the Stoic, I journal, I read 10 pages of a non-fiction book. And then I start my day, I go to the gym regularly. And when I don't do these things, I notice a big difference in my overall wellbeing as far as how I attack the day and how I approach others. This is from Jim Quick- who says that your brain is a muscle and you have to continue to work it. By reading every day or doing puzzles, you're working that muscle and continuing to develop it just like you would your body (read Limitless by Jim Quick).
*For more information or additional links to the wisdom of JESI STRACHAM, please visit:
Disclaimer
& Copyright Notice: The materials provided on this website/web-based
article are copyrighted 2022 and the intellectual property of the publishers/producers
(The NY Cancer Resource Alliance/IntermediaWorx inc and the AngioFoundation
(501c3). It is provided publicly strictly for informational purposes within
non-commercial use and not for purposes of resale, distribution, public display
or performance. Unless otherwise indicated on this web based page, sharing,
re-posting, re-publishing of this work is strictly prohibited without due
permission from the publishers. Also,
certain content may be licensed from third-parties. The licenses for some of this
content may contain additional terms. When such Content licenses contain
additional terms, we will make these terms available to you on those pages
(which his incorporated herein by reference). This feature content and the
digital platforms this resides in does not support, endorse or recommend any
specific products, tests, physicians, procedures, treatment opinions or other
information that may be mentioned on this site. Referencing any content or
information seen, published or shared by other individuals is solely at your
own risk. The publishers/producers of this article reserves the right, at its
sole discretion, to modify, disable access to, or discontinue, temporarily or
permanently, all or any part of this Internet web site or any information contained
thereon without liability or notice to you.












No comments:
Post a Comment